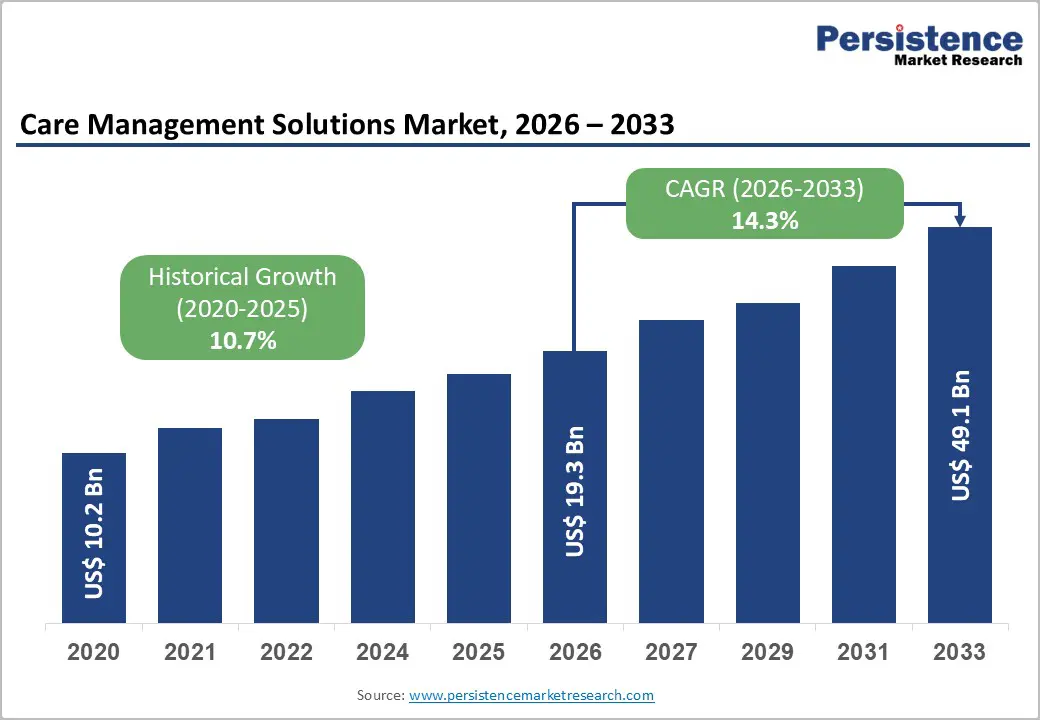
The global healthcare landscape is undergoing a profound transformation, driven by rising chronic disease burdens, aging populations, and a growing emphasis on patient-centric care. At the heart of this evolution lies the Care Management Solutions Market, a rapidly expanding segment that is redefining how healthcare providers coordinate, monitor, and optimize patient care.
According to recent projections, the Care Management Solutions Market is expected to grow from US$19.3 billion in 2026 to US$49.1 billion by 2033, registering a robust CAGR of 14.3%. This growth reflects the increasing need for integrated platforms that enable continuous care, reduce hospital readmissions, and support value-based healthcare models.
Understanding Care Management Solutions
Care management solutions are digital platforms and services designed to streamline patient care coordination across multiple healthcare providers, settings, and timeframes. These solutions integrate clinical, administrative, and financial data to support:
- Chronic disease management
- Remote patient monitoring
- Population health management
- Care coordination and communication
- Predictive analytics and decision support
By centralizing patient information and enabling real-time insights, these tools empower healthcare organizations to deliver more efficient and personalized care.
Key Market Drivers Fueling Growth
Rising Prevalence of Chronic Diseases
One of the most significant drivers of the care management solutions market is the increasing global burden of chronic diseases such as diabetes, cardiovascular conditions, COPD, and hypertension. These conditions require long-term monitoring, frequent interventions, and coordinated care across multiple providers.
Care management platforms play a critical role in addressing these challenges by:
- Enabling continuous patient monitoring through remote devices
- Supporting medication adherence and care plans
- Facilitating timely interventions to prevent complications
Studies indicate that AI-enabled remote monitoring can reduce hospital readmissions by 25–50%, highlighting the clinical and economic value of these solutions.
Shift Toward Value-Based Care Models
Healthcare systems worldwide are transitioning from traditional fee-for-service models to value-based care, where providers are rewarded for patient outcomes rather than service volume.
Care management solutions are essential in this shift, as they help:
- Identify high-risk patients through predictive analytics
- Coordinate care across multidisciplinary teams
- Track performance metrics and outcomes
- Reduce unnecessary hospital utilization
For instance, over 53% of Traditional Medicare beneficiaries are now part of accountable care arrangements, emphasizing the growing importance of coordinated care delivery systems.
Market Restraints and Challenges
Interoperability and Legacy System Barriers
Despite strong demand, the adoption of care management solutions faces challenges due to fragmented healthcare IT systems. Many electronic health record (EHR) systems operate in silos, limiting seamless data exchange.
Key issues include:
- Lack of standardized data formats
- High costs of integrating legacy systems
- Complex implementation processes
These barriers increase the total cost of ownership and delay deployment timelines, particularly for smaller healthcare providers.
Data Privacy and Regulatory Complexity
Care management solutions rely heavily on sensitive patient data, making data privacy and security a critical concern. Compliance with regulations such as HIPAA and other regional frameworks requires:
- Advanced encryption and cybersecurity measures
- Role-based access controls
- Comprehensive audit trails
These requirements can increase operational complexity and costs, potentially slowing market adoption.
Emerging Opportunities in the Market
Integration of AI and Predictive Analytics
Artificial intelligence (AI) is revolutionizing care management by enabling data-driven clinical decision-making. AI-powered platforms can:
- Automate administrative tasks such as documentation
- Predict patient risks and disease progression
- Personalize treatment plans
- Enhance patient engagement
For example, AI-enabled care management tools have demonstrated:
- 28% reduction in documentation time
- 20% increase in patient engagement
These advancements are making healthcare delivery more efficient and proactive.
Expansion of Remote Patient Monitoring and Telehealth
The rapid adoption of telehealth and remote patient monitoring (RPM) is significantly expanding the scope of care management solutions. With the integration of IoT devices and mobile health applications, providers can:
- Monitor patients in real time from their homes
- Detect early signs of deterioration
- Improve medication adherence
- Reduce hospital visits
This trend is particularly important in regions with limited healthcare access, where digital solutions can bridge gaps in care delivery.
Category-Wise Market Analysis
Solution Segment: Software Leads the Way
The software segment dominates the market, accounting for over 65% share in 2026, valued at more than US$12.5 billion. This dominance is driven by the need for:
- Centralized patient data management
- Real-time analytics and reporting
- Care coordination and workflow automation
Meanwhile, the services segment is the fastest-growing, fueled by demand for:
- Implementation and integration
- Training and support
- Consulting and managed services
As healthcare systems become more complex, service providers play a crucial role in ensuring successful adoption and utilization.
Deployment Segment: On-Premises vs Cloud
On-premises solutions currently hold over 35% market share, preferred by large healthcare organizations for:
- Enhanced data control and security
- Integration with existing IT infrastructure
- Regulatory compliance
However, cloud-based solutions are witnessing the fastest growth due to:
- Scalability and flexibility
- Lower upfront costs
- Rapid deployment capabilities
- Support for remote care and telehealth
The shift toward cloud adoption reflects the broader digital transformation in healthcare.
End User Segment: Hospitals Lead, Home Healthcare Rising
Hospitals and clinics dominate the market with over 38% share, driven by:
- Complex patient populations
- Need for coordinated care delivery
- Pressure to reduce readmissions
- Adoption of value-based care models
On the other hand, home healthcare providers represent the fastest-growing segment. This growth is fueled by:
- Aging populations
- Rising demand for home-based care
- Cost-effective treatment alternatives
- Increased use of remote monitoring technologies
Regional Insights
North America: Market Leader
North America holds the largest market share, accounting for over 39% in 2026, with a value of approximately US$7.5 billion. Growth in this region is supported by:
- Advanced healthcare infrastructure
- High IT spending
- Strong regulatory frameworks
- Widespread adoption of digital health technologies
The United States leads the region, driven by Medicare and Medicaid initiatives promoting value-based care.
Asia Pacific: Fastest-Growing Region
Asia Pacific is expected to register the highest growth rate, with a CAGR of 19.6%. Key growth drivers include:
- Rapid digital health adoption
- Government initiatives in countries like China, India, and Japan
- Expansion of telehealth services
- Rising chronic disease prevalence
India, in particular, is emerging as a key market due to its digital health ecosystem and increasing investments in healthcare infrastructure.
Europe: Strong Growth Potential
Europe accounts for over 20% market share, supported by:
- Aging populations
- National eHealth initiatives
- Improved interoperability through regulatory frameworks
Countries like Germany, the UK, and the Netherlands are leading adoption, with strong emphasis on digital transformation and care coordination.
Competitive Landscape and Key Players
The care management solutions market is moderately consolidated, with major players focusing on innovation, partnerships, and acquisitions to strengthen their market position. Leading companies include:
- Epic Systems Corporation
- Cerner Corporation
- Allscripts Healthcare Solutions
- Cognizant Technology Solutions
- IBM Corporation
- Koninklijke Philips N.V.
- Salesforce, Inc.
- Optum, Inc.
These companies are investing heavily in AI integration, interoperability, and platform consolidation to meet evolving healthcare needs.
Recent Industry Developments
Recent innovations highlight the growing role of AI and automation in care management:
- In April 2025, Innovaccer launched AI-powered copilots to automate documentation and patient engagement processes.
- HealthEdge introduced an AI-driven provider data management platform to enhance data accuracy and compliance across healthcare networks.
Such advancements are accelerating the adoption of intelligent care management systems.
Future Outlook: What Lies Ahead?
The future of the care management solutions market looks promising, with several trends shaping its trajectory:
- Increased AI adoption for predictive and personalized care
- Expansion of telehealth and remote monitoring ecosystems
- Greater interoperability through standardized data frameworks
- Focus on patient-centric care models
- Rising investments in digital health infrastructure
As healthcare systems continue to evolve, care management solutions will play a pivotal role in improving patient outcomes, reducing costs, and enhancing operational efficiency.
Conclusion
The care management solutions market is at the forefront of healthcare transformation, driven by the need for better care coordination, improved patient outcomes, and cost efficiency. With strong growth projections and continuous technological advancements, the market is poised to become a cornerstone of modern healthcare systems.
Organizations that invest in integrated, AI-driven care management platforms will be better positioned to navigate the complexities of value-based care and deliver high-quality, patient-centric services in the years ahead.