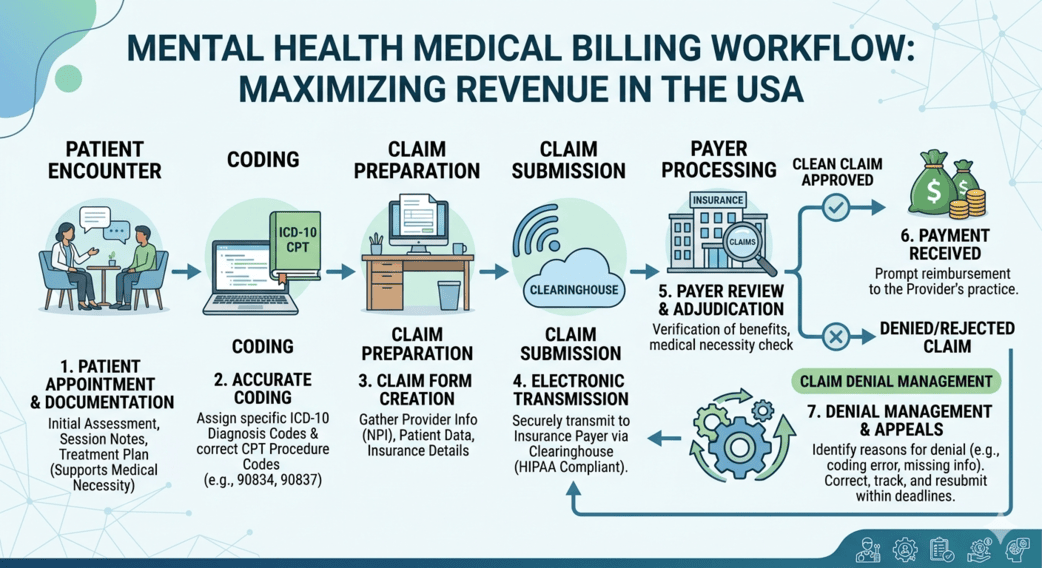
The demand for behavioral and psychiatric care across the United States has grown rapidly over the last few years. From private therapists and psychologists to large mental health clinics, providers are seeing more patients than ever before. But while patient volume increases, administrative pressure grows alongside it.
Insurance verification delays, denied claims, coding mistakes, and credentialing bottlenecks are now among the biggest challenges affecting mental health practices. That’s why many providers are turning to professional mental health billing and credentialing services to stabilize revenue, reduce errors, and improve patient experience.
For therapists and behavioral health organizations, billing is no longer just an administrative task. It directly affects cash flow, compliance, provider reputation, and operational efficiency.
The Growing Complexity of Mental Health Billing
Mental health reimbursement is more complicated than many other medical specialties. Behavioral health providers often deal with:
- Time-based CPT codes
- Telehealth billing rules
- Frequent insurance authorization requirements
- Modifier usage
- Evolving payer policies
- Session documentation audits
- Medicaid and Medicare compliance
Even experienced clinics struggle to manage these complexities internally. A single coding error or missing authorization can delay payments for weeks.
This is where mental health insurance billing services become essential. Dedicated specialists understand behavioral health coding rules and payer-specific guidelines, helping providers avoid costly denials.
Why Credentialing Is Critical for Mental Health Practices
Before providers can even bill insurance companies, they must complete payer enrollment and credentialing processes. Unfortunately, credentialing delays are common in behavioral healthcare.
A therapist may wait several months before being approved by major insurance carriers. During that period, practices often lose potential revenue opportunities.
Professional credentialing services help providers:
- Complete enrollment paperwork accurately
- Track application status
- Avoid missing documentation
- Revalidate provider credentials on time
- Maintain payer compliance
Without proper credentialing, even correctly submitted claims can be rejected.
What Mental Health Billing and Credentialing Services Actually Include
Many providers assume billing companies only submit claims. In reality, a full-service mental health billing services agency handles far more than that.
Typical services include:
Insurance Eligibility Verification
Before appointments are scheduled, billing teams verify:
- Active coverage
- Copays
- Deductibles
- Authorization requirements
- Telehealth eligibility
This reduces unexpected denials and improves patient transparency.
Behavioral Health Coding
A qualified mental health billing specialist understands psychotherapy coding, evaluation and management services, group therapy billing, and crisis intervention codes.
Accurate coding is critical because behavioral health claims are heavily scrutinized by payers.
Claims Submission and Tracking
A professional mental health billing provider ensures claims are submitted correctly and followed through until payment is received.
This includes:
- Electronic claim filing
- Clearinghouse management
- Rejected claim correction
- Payment posting
- Accounts receivable follow-up
Denial Management
Denied claims can significantly affect practice revenue. Experienced billing teams investigate denial causes and resubmit corrected claims quickly.
Many practices discover that denial rates decrease substantially after partnering with a dedicated mental health billing agency.
Credentialing and Provider Enrollment
Credentialing specialists handle payer enrollment, CAQH maintenance, and recredentialing requirements for therapists, psychiatrists, psychologists, and counselors.
Why Providers Choose to Outsource Mental Health Billing Services
Hiring and training an in-house billing team is expensive. Mental health practices also face staffing shortages and employee turnover, which can disrupt revenue cycles.
As a result, many organizations now outsource mental health billing services to experienced healthcare revenue experts.
Outsourcing offers several advantages.
Reduced Administrative Burden
Therapists and clinicians can focus on patient care instead of insurance paperwork.
Faster Reimbursements
Experienced billing teams know how to prevent claim errors before submission, improving payment turnaround time.
Better Compliance
Behavioral health regulations continue to evolve. Outsourced teams stay updated on payer policies and industry changes.
Lower Operational Costs
Maintaining internal billing departments requires salaries, software, training, and compliance management. Outsourcing often costs less while improving efficiency.
Access to Specialized Expertise
A professional mental health billing consultant understands payer behavior, coding changes, and reimbursement trends unique to behavioral healthcare.
Common Challenges Mental Health Providers Face
Even successful clinics encounter billing obstacles that affect profitability.
Frequent Claim Denials
Behavioral health claims are often denied due to:
- Missing modifiers
- Incorrect session durations
- Authorization issues
- Documentation gaps
A knowledgeable mental health billing and coding company can significantly reduce denial rates.
Telehealth Billing Confusion
Virtual therapy expanded rapidly, but telehealth reimbursement policies continue changing across states and insurance carriers.
Providers must stay updated on:
- Place of service codes
- Telehealth modifiers
- State licensing rules
- Audio-only billing regulations
Delayed Credentialing
Many mental health providers experience payer enrollment delays lasting several months. Without expert support, these delays can disrupt revenue and patient onboarding.
Insurance Follow-Up Delays
Mental health practices often lack time to follow up on aging claims. This results in unpaid balances accumulating over time.
The Role of Technology in Modern Mental Health Billing
Today’s leading mental health medical billing solution providers use advanced billing platforms and automation tools to improve efficiency.
Technology helps practices:
- Track claims in real time
- Identify denial trends
- Automate payment posting
- Improve reporting accuracy
- Reduce manual errors
However, software alone is not enough. Human expertise remains essential because behavioral health billing rules frequently change.
That’s why many clinics prefer working with a hybrid solution combining technology and experienced billing professionals.
How the Best Mental Health Billing Agency Supports Practice Growth
The right billing partner does more than process claims. They help practices scale sustainably.
A reliable best mental health billing agency often provides:
- Financial reporting insights
- Revenue optimization strategies
- Payer contract analysis
- Workflow improvements
- Compliance monitoring
For growing practices, these services can make a major difference in long-term profitability.
What to Look for in a Mental Health Billing Company
Not all billing providers specialize in behavioral health. Choosing the wrong partner may create more problems than solutions.
When evaluating mental health billing companies, consider the following factors.
Industry Experience
Behavioral health billing differs significantly from general medical billing. Look for teams with mental health expertise.
Transparent Reporting
Practices should receive regular updates on:
- Claim status
- Collections
- Denials
- Accounts receivable
Credentialing Support
The ideal partner should also provide integrated credentialing services.
Compliance Knowledge
Mental health records and claims involve strict HIPAA and payer compliance requirements.
Scalability
As practices grow, billing support should scale with them.
Benefits of Mental Health Medical Billing Services Outsourcing
More providers are adopting mental health medical billing services outsourcing because it allows them to stay competitive without expanding internal administrative teams.
Outsourcing can improve:
- Cash flow consistency
- Provider productivity
- Patient satisfaction
- Revenue visibility
- Administrative efficiency
For independent therapists and group practices alike, the financial impact can be substantial.
Real-World Example: How Outsourced Billing Improved Collections
A mid-sized therapy group in Dallas struggled with a 28% claim denial rate due to inconsistent coding and delayed insurance follow-ups.
After transitioning to an outsourced mental health billing model, the practice implemented:
- Dedicated denial management
- Real-time eligibility verification
- Automated claim tracking
- Behavioral health coding audits
Within six months:
- Denials dropped significantly
- Average reimbursement turnaround improved
- Outstanding accounts receivable decreased
- Providers spent less time on administrative tasks
This type of improvement is becoming increasingly common as practices work with specialized billing experts.
Why Billing Services for Mental Health Therapists Are Different
Therapists face unique billing challenges compared to other healthcare providers.
Session lengths vary, treatment plans require detailed documentation, and payer rules frequently change. In addition, many therapists balance self-pay clients with insurance billing.
That’s why specialized billing services for mental health therapists focus specifically on psychotherapy workflows rather than general medical claims.
These services often include:
- Session-based coding support
- Teletherapy billing
- Insurance eligibility verification
- Copay collection guidance
- Documentation review
The Importance of Revenue Cycle Management Services
Behavioral health practices cannot rely solely on claim submission. A complete financial strategy requires strong revenue cycle management services.
Revenue cycle management covers every stage of the payment process, including:
- Patient registration
- Insurance verification
- Coding
- Claim submission
- Payment posting
- Denial management
- Patient collections
- Financial reporting
When managed properly, revenue cycle optimization improves both profitability and operational stability.
Why Medical Coding Services Matter in Behavioral Health
Coding errors remain one of the leading causes of denied mental health claims.
Professional medical coding services help practices:
- Apply accurate CPT and ICD-10 codes
- Reduce audit risk
- Improve reimbursement accuracy
- Maintain payer compliance
Behavioral health coding requires detailed understanding of psychotherapy documentation standards, especially for longer sessions and crisis intervention billing.
The Value of Integrated Medical Billing and Coding Services
Many providers now prefer combined medical billing and coding services instead of managing coding separately.
Integrated services improve communication between coders and billing specialists, reducing delays and improving first-pass claim acceptance rates.
This approach also helps practices identify recurring documentation problems before they affect reimbursements.
How Professional Mental Health Billing Companies Improve Patient Experience
Billing affects patients more than many providers realize.
Confusing invoices, delayed insurance processing, and inaccurate balances can damage trust and satisfaction.
A professional mental health billing company improves patient experience by:
- Verifying benefits before visits
- Explaining financial responsibilities clearly
- Reducing billing disputes
- Processing claims efficiently
This creates a smoother experience for both patients and providers.
Choosing the Top Outsource Mental Health Billing Company
Finding the top outsource mental health billing company requires careful evaluation.
Providers should prioritize companies that offer:
- Behavioral health specialization
- Transparent communication
- Dedicated account management
- Strong reporting systems
- HIPAA compliance
- Credentialing expertise
- Proven denial reduction strategies
The goal is not simply outsourcing tasks but building a long-term revenue partnership.
Supporting Practice Growth with the Right Billing Partner
As mental health demand continues rising across the United States, providers need operational systems that support sustainable growth.
Partnering with experienced professionals for:
- medical billing services
- medical coding services
- medical billing and coding services
- revenue cycle management services
- credentialing services
can help practices improve financial performance while reducing administrative strain.
Many healthcare organizations now rely on trusted industry partners like 247 Medical Billing Services to streamline behavioral health billing operations without compromising patient care quality.
Conclusion
The financial side of behavioral healthcare has become increasingly complex. From insurance verification and coding to credentialing and denial management, mental health providers face constant administrative challenges that can directly impact revenue.
Professional mental health billing and credentialing services help practices reduce errors, accelerate reimbursements, improve compliance, and create a better patient experience.
Whether you operate a private therapy office or a large behavioral health clinic, partnering with an experienced mental health billing services agency can provide the operational support needed to grow confidently in today’s competitive healthcare environment.
As the industry evolves, practices that invest in specialized billing expertise will be better positioned to maintain financial stability while focusing on what matters most — patient care.
FAQs
What are mental health billing and credentialing services?
Mental health billing and credentialing services help behavioral healthcare providers manage insurance claims, coding, payer enrollment, denial management, and reimbursement processes efficiently.
Why should providers outsource mental health billing services?
Many practices outsource billing to reduce administrative workload, improve claim accuracy, accelerate reimbursements, and access specialized behavioral health expertise.
How does credentialing affect mental health reimbursement?
Without proper credentialing, insurance companies may reject claims or delay payments. Credentialing ensures providers are approved to bill payers legally and correctly.
What does a mental health billing specialist do?
A mental health billing specialist handles psychotherapy coding, claim submission, insurance follow-ups, denial management, and payment tracking for behavioral health practices.
Are mental health billing companies HIPAA compliant?
Reputable mental health billing companies follow strict HIPAA regulations to protect patient information and maintain compliance standards.
What should I look for in the best outsource mental health billing and coding company?
Look for behavioral health experience, transparent reporting, credentialing support, denial management expertise, compliance knowledge, and strong client communication.